Background and Objectives: Scrub typhus is grossly under-diagnosed in India due to its non specific clinical presentation, limited awareness and low index of suspicion among clinicians, and lack of diagnostic facilities. As there is a resurgence of scrub typhus in this part of north Karnataka, an attempt is made to study the clinical prolife and complications of scrub typhus in adult patients. Materials and Methods: All cases of febrile illness diagnosed as scrub typhus over a period of 1 year were analysed. Diagnosis was based on the presence of the eschar and /or positive Weil Felix test with a titre of > 1:80. Results: 50 patients diagnosed to have scrub typhus during study period of one year were included in the study. Headache, myalgia, nausea, vomiting and dry cough were common symptoms. More than half of the patients had fever of 7-14 days duration (54%). Eschar was seen only in six patients. Transaminitis was noted in 86.67% patients. Weil Felix test was positive in 48/50 patients with titers of 1:160 in 13 patients, 1:320 in 31 patients and 1:640 in 4 patients. In our study complications noted were acute renal failure (07cases), ARDS and encephalitis 04 cases each and septic shock 01 case. Conclusion: There is a resurgence of scrub typhus in this part of north Karnataka, as one of the important cause of acute febrile illness. Weil Felix test serves as a useful and cheap test for the laboratory diagnosis of Rickettsial disease. Keywords: Eschar, scrub typhus, Weil-Felix test
Scrub typhus is an acute febrile illness caused by Rickettsia tsutsugamushi. [1] Scrub typhus or tsutsugamushi disease is widely endemic in Indian subcontinent. [2] Worldwide, more than one million cases occur annually and as many as one billion people living in endemic areas may have been infected at some time. [3] Many studies from India, particularly from south India have reported outbreak/isolated reports of scrub typhus in the past. [2] Although, a seasonal outbreak of cases of fever is being reported continuously for the last few years from this region of north Karnataka, but the disease remained undiagnosed or underdiagnosed. Recent reports from several parts of India, including south India, indicate that there is a resurgence of scrub typhus. [4],[5],[6] Scrub typhus is grossly underdiagnosed in India due to its nonspecific clinical presentation, limited awareness and low index of suspicion among clinicians, and lack of diagnostic facilities. The infection manifests clinically as a nonspecific febrile illness often accompanied by headache, myalgia, nausea, vomiting, diarrhea, cough, or breathlessness. Severity varies from subclinical illness to severe illness with multiple organ system involvement, which can be serious enough to be fatal, unless diagnosed early and treated. [1] With improvement in existing diagnostic methods, advances in epidemiology, and advent of new diagnostic kits, the control of rickettsial infections appears to be an achievable task. As there is a resurgence of scrub typhus in this part of north Karnataka, an attempt is made to study the clinical prolife and complications of scrub typhus in adult patients.
All patients of age ≥15 years with acute febrile illness admitted in medicine wards during March 2011 to April 2012 were included in the study. Detailed history, clinical examination including careful search for eschar was made in all the patients and investigations mentioned below were done. The results were analyzed and descriptive statistics was used. Inclusion criteria 1) Age of patients more than or equal to 15 years. 2) Patients diagnosed to have scrub typhus on the basis of eschar and/or positive Weil-Felix test were included in the study. Data was collected by using proforma meeting the objectives of the study. Purpose of the study was carefully explained to the patients and informed consent was taken. Investigations Complete hemogram, blood urea, serum creatinine, urine routine, urea, creatinine, random blood sugar, and liver function tests were done in all these patients. To establish the cause of fever, additional investigations including blood culture, chest X-ray, widal, rapid card test for malarial antigen, serology for leptospirosis, serology for dengue, ultrasonography (USG) abdomen, and urine culture were also done in majority of patients. In addition, Weil-Felix test was done in all these patients. Statistical software The statistical software namely SPSS 15.0, STATA 8.0, MEDCALC 9.0.1, and SYSTAT 11.0 were used for analysis of data and Microsoft Word and Excel have been used to generate the graphs and tables.
Fifty patients diagnosed to have scrub typhus during study period of 1 year were included in the study. Out of 50 patients of scrub typhus diagnosed, 31 were males and 19 were females. The age of patients varied from 18-90 years. Most of the patients were from rural areas of Dharwad and nearby districts. Maximum numbers of cases were seen during September month. [Table 1] shows clinical presentation of scrub typhus. Headache, myalgia, nausea, vomiting, and dry cough were common symptoms. More than half of the patients had fever for 7-14 days (54%). Most common signs in this study were hepatomegaly, splenomegaly, and lymphadenopathy. Eschar was seen only in six patients. Eschar was noted over the abdomen (infraumbilical: 4, supraumbilical: 1, and thigh: 1).
[Table 2] shows laboratory investigations of scrub typhus patients. Twenty-one patients had total leukocyte count >11,000 per mm 3 and 32 (62%) patients had thrombocytopenia (platelets < 1.5 lakhs). Transaminitis was noted in 86.67% patients.
Weil-Felix test was positive in 48/50 patients with titers of 1:160 in 13 patients, 1:320 in 31 patients, and 1:640 in four patients. In two patients, diagnosis of scrub typhus was made on eschar alone with Weil-Felix test being negative in these patients. [Table 3] shows complications of scrub typhus. Nearly two-third of our patients had thrombocytopenia and hepatic dysfunction (↑ bilirubin or ↑ SGOT/SGPT or ↑ ALP) as most common complications. Four patients expired in our study and mode of death in all of them was acute multiorgan failure.
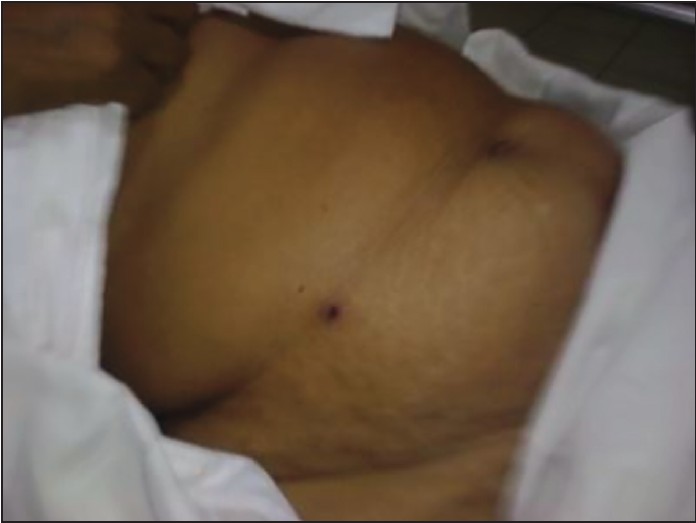
Scrub typhus or tsutsugamushi disease is widely endemic in the Indian subcontinent. [2] Over the last decade, most of the acute febrile illness remained undiagnosed or underdiagnosed for scrub typhus due to its difficulty in diagnosis, because of its nonspecific clinical presentation, low index of suspicion and absence of advanced laboratory diagnostic techniques in our setup. Recently several reports of scrub typhus from various parts of India have been published. [4],[5],[6] Age and sex are known to influence the occurrence of scrub typhus mainly due to the exposure and inclination of outdoor activities whether occupational or recreational. [2] Most of the cases belonged to age group of 26-50 years. Two-third of the patients was men and this may be due to their outdoor activities. Ogawa et al., [3] did not note any sex influence on the distribution of cases. Further epidemiological studies are required to substantiate this point. Most of cases (30%) were seen during September month resembling autumn-winter type scrub typhus. Similar seasonal distribution has been established from Jammu in a study by Mahajan et al. [2] The clinical course of the disease and prognosis vary depending on the character of endemic strain. These variations in clinical presentations and severity are very much evident in the studies from different parts and at different times from world as well as India. [2] Most of the cases in our study presented with nonspecific symptoms localizing to respiratory or gastrointestinal tract. Unlike the usual viral illnesses, the duration of fever in majority of cases is usually more than 7 days. In addition to myalgia and headache; nausea, vomiting, cough, and breathlessness were seen in a significant number of cases [Table 1]. Eschar at the site of attachment of larval mite or chigger, is the most characteristic feature of scrub typhus, but not seen in all patients. Eschar is a black necrotic lesion resembling a cigarette burn usually found in areas where skin is thin, moist, or wrinkled and, where the clothing is tight [Figure 1], [Figure 2], and [Figure 3]. In our study eschar was found in seven out of 50 cases. The most common site involved was abdomen. Often patients were not aware of the presence of eschar, as it hardly produced any symptoms of discomfort. The presence of an eschar is though, highly suggestive of scrub typhus but is reported to occur in a variable proportion of patients in various studies. Thus, its presence confirms and is path gnomic of the disease but its absence does not exclude the possibility of scrub typhus. Indian studies by Mathai et al., [4] Vivekanandan et al., [1] and Mahajan et al., [7] reported an incidence of eschar as 4, 46, and 10% of cases, respectively.
Eschar is usually associated with regional lymphadenopathy and sometimes generalized lymphadenopathy. Lymphadenopathy was found in 22% of the cases in our study and this is consistent with observations in other studies. In India, Mahajan et al., [7] found it in 53% of the cases while Vivekanandan et al., [1] and Mahajan et al., [2] from Jammu noted it in 30 and 45% of the cases, respectively. Among the laboratory parameters, the most consistent abnormality noticed was transaminitis which was present in 86.67% of our cases [Table 2]. Similar abnormalities have been observed by Mathai et al., [4] and Vivekanandan et al., [1] in their studies. In our study 96% cases found to have Weil-Felix test positive with titer of ³1:160. Mathai et al., [4] and Vivekanandan et al., [1] in their studies found Weil-Felix test to be positive in 77 and 78%, respectively. Weil Felix test has not been found to be a sensitive test to detect scrub typhus in the community by other studies, but when positive, it is highly specific. According to Issac et al., [8] from Christian Medical College, Vellore, specificity of the test is high, even at a titer as low as 1/20. Hence, they suggested that patients with low titers also should be evaluated for scrub typhus. However, the test lacks sensitivity. Specific immunological tests like, immunoflourescent antibody test (IFA) immunoperoxidase test (IIP), etc. are costly and are not available in our country. Weil-Felix test serves as a useful and cheap test for laboratory diagnosis of Rickettsial disease, as has been proven in several areas around the world. [1] Scrub typhus is known to produce serious complications and has a mortality rate of 7-30%. [9],[10] Deaths are attributable to late presentation, delayed diagnosis, and drug resistance. In our study, complications noted were acute renal failure (seven cases), acute respiratory distress syndrome (ARDS) and encephalitis (four cases each), and septic shock (01 case). Similar observations were noted by Pandey et al., [9] from Himachal Pradesh (three cases of ARDS) and Tsay et al., [11] from Taiwan found eight cases of ARDS, three cases of acute renal failure, and one case each of myocarditis and septic shock. The limitation of the present study is that the diagnosis of scrub typhus was made only on the basis of Weil-Felix test and/or the presence of eschar and specific immunoglobulin M (IgM) antibodies were not done.
A high degree of clinical suspicion and familiarity with various clinical manifestations is essential for early diagnosis of scrub typhus. There is a reemergence of scrub typhus in this part of Karnataka and demands early diagnosis and timely initiation of appropriate therapy, thereby reducing patient morbidity and mortality. Weil-Felix test serves as a useful economical tool for laboratory diagnosis of scrub typhus where confirmatory tests are not available.
Source of Support: None, Conflict of Interest: None
[Figure 1], [Figure 2], [Figure 3]
[Table 1], [Table 2], [Table 3] |
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||