Background: Circumcision practice around the world has various implications and has generated a lot of debate about the pros and cons of the practice. Nigeria is one of the countries where male and female circumcision practice still occurs however, there has been claim of reduction in female genital cutting. Congregational or ‘group’ circumcision prevails in some communities as a means of upholding traditions and commemoration of festive period. Objective: To determine the pattern of circumcision practice and identify factors affecting the practice in Ilorin community. Materials and Methods: The study was a descriptive, cross sectional study conducted among parents of under-5 children of both the sexes using pre-tested, semi-structured questionnaires, which were administered to the respondents by trained research assistants over a six-week period. Clinical examination of genital area in index child of each respondent was done by a pediatric surgeon, who was the principal investigator. Results: Three hundred and ninety three (93%) respondents completed the questionnaire and the same number of index children’s external genitalia was examined by the pediatric surgeon. The mean age of respondents was 33.2±9.3 years, and the main source of family income was private enterprises and civil services. The circumcision status of fathers was 100%, mothers, 65.6%, and overall female-child circumcision rate was 46.7%. Though, most of the index children were delivered at health centers (72.3%), the circumcisions were performed at almost equal frequencies by traditional circumcisionists (39.8%) and doctors (39.2%), with more than half of the circumcision being done outside the hospital. The mean age at circumcision was 22 ±0.69 months, with 73.9% of girls as against 91.7% boys being circumcised by the age of five years. Family choice was the main determinant of the age at circumcision and the circumcisionist. Female circumcision was done by traditional circumcisionist, nurses, and doctors in 1 in 4, 1 in 5, and 1 in 10 cases of circumcision, respectively. Traditional open (classical) circumcision technique was mostly used (40.4%), followed by Plastibel TM (ring type) (32.6%), and ‘group’ circumcision was practiced among 41.2% of respondents. Post-circumcision complications were seen in 116 (33.7%) of circumcised children examined. Conclusion: Circumcision practice in Ilorin is still higher among the traditional circumcisionists, despite of high hospital delivery. Female circumcision and ‘group’ circumcision were also being practiced, using mainly the traditional open circumcision technique. The high rate of circumcision complications indicate the need for proper enlightenment and retraining of health care providers and traditional circumcisionists on the safe methods available. The government should involve the religion and opinion leaders in the community to assist in the prevention of negative and harmful traditional practices including female circumcision. Keywords: Circumcision, community practice, female circumcision, group circumcision
Circumcision has been widely practiced from the immemorial time, around the world, for different reasons and at different stages of life. Health promotion and health protection are medical reasons given in the developed world for circumcision. In many developing countries, such as Africa and Asia, cultural, religious, and aesthetic reasons are given. [1] About one-third of the world’s male population has been circumcized. [2] Many reports have reappraised the indications for circumcision, and others have highlighted the alternatives of circumcision. [3] Circumcision is currently claimed to give protection against HIV infection, and wide male circumcision is advocated. [4],[5] In sub-Saharan Africa, female circumcision, and especially infibulation or pharaonic circumcision is performed, despite of the complications associated with it. In a national survey across the 36 states of Nigeria, the prevalence of female genital cutting (FGC) was highest in: Ekiti (89%), Edo (88%), Ondo and Kwara (83%), Ebonyi (76%), and Bayelsa (72%) with a national prevalence rate of 40%. [6] Traditionally, circumcision for the male is regarded as an educational institution which prepares them for courtship, negotiating marriage, and other social responsibilities; while for the female, it is a mean of curbing promiscuity. [7],[8] The settings and practitioners of circumcision vary in different communities and countries. ‘Group circumcision’ during festive periods is a common practice in Nigeria. Complications arising from circumcision are often concealed for life either due to death of the victims or fear of being made an outcast by the society. [9] This study aimed at documenting the pattern of circumcision practice and identifies factors affecting the practice in Ilorin community in the northern part of Nigeria.
The study was carried out between January 15 th and February 29 th 2008 in Ilorin, an ancient and political capital of Kwara state. It is the gate way between the southern and northern part of Nigeria, and currently in the North-central geopolitical zone. The people are mainly Yorubas and muslims, but there is a mix of other tribes and religion because of its location. The 2006 census, which is the most recent, put the population at 786,429, with an estimated annual population growth rate of 2.5%. [10] The economy of the area is mostly pre-industrial, with the major occupation of the people being peasant farming and cloth weaving. The educated citizens are employed in the civil service, and a sizeable number of the population is engaged in commerce, and small scale industrial enterprises. The study was a descriptive, cross sectional study conducted among mothers of under-5 children of both the sexes using pre-tested, semi-structured questionnaires, which were administered to the respondents by trained research assistants. The pediatric surgeon conducted the clinical examination of genital area in the index child of each respondent. A multi-staged sampling technique was used to select the household, and index child was randomly selected among the circumcized children in the household. The sample size was calculated with Fisher’s formula, and by allowing for a 10% attrition rate, a total sample size of 422 was estimated. Multistage sampling technique was used to select the subjects from households in compounds of various wards. Due consent was obtained from the household head and respondents after explaining the objectives of the study and confidentiality of findings was ensured. Data were analyzed using the Statistical Package for Social Sciences (SPSS) software version 11.0 and Microsoft Excel for Windows 2007.
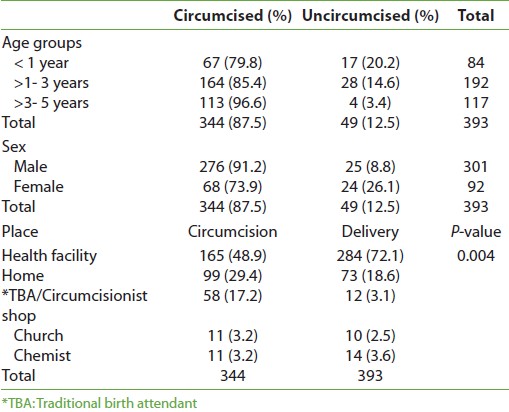
Three hundred and ninety three respondents made up, mainly of 287 mothers (73%), 95 (24.7%) fathers, and 11 (2.8%) caregivers, living in the household and completed the questionnaires. The religions were Islam, 324 (82.4%), Christianity, 59 (15%), and native traditional religion, 10 (2.6%). The respondents ethnic groups were Yorubas (346, 86%), Hausa (8, 2%), Fulani (15, 4%), Igbos (7, 2%), and Nupe, Tapa, Gobirs (25, 6%). The age of respondents ranged between 17 years and 70 years with a mean of 33.2 ± 9.3. Most of the respondents were in the 21- 40 years age group [Table 1]. The age groups of index children are as shown in [Table 1], with almost half of them in age group one to three years, 192 (48.9%). The male: female ratio was 3:1 among the index children.
Almost equal numbers of mothers (178, 45.2%) and fathers (185, 47.3%) had minimum of secondary level education, but education level was not known in 15.8% and 37% of mothers and fathers, respectively. The occupation of respondents included trading 151 (37.4%), civil service 111 (28.2%), while 48 (12.2%) were unemployed [Table 1]. The fathers, mothers, and other respondents were circumcized in 100%, 65.6%, and 100% of situation, respectively. Place of delivery of majority of the index children was in a hospital (284, 72.3%) and in other places as shown in [Table 2]. However, the circumcisions were performed at almost equal frequencies by traditional circumcisionists (39.8%) and doctors (39.2%), followed by nurses (17.2%), chemists (1.7%), and others (2.1%) in the study [Table 3].
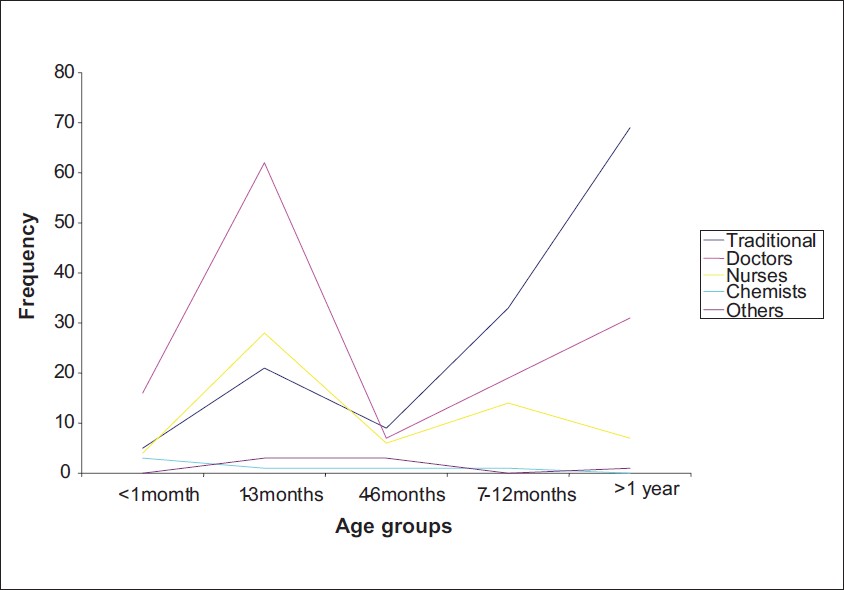
The overall circumcision status of the index children was 87.5%, and the older the child is, the more likely that circumcision has taken place [Table 2]. However, 73.9% of the girls as against 91.7% boys recruited in the study have been circumcized by the age of five years. More than half of the circumcisions were done outside the hospital [Table 2]. About 1 in 4 cases of circumcision done by traditional circumcisionist is a female circumcision, while about 1 in 10 circumcisions by doctors were on the female. The nurse did 1 in 5 circumcisions, on the female, as shown in [Table 3]. The lower age groups were circumcized by the health practitioners (doctors and nurses), while the older age circumcisions (> 1 year) were done by traditional circumcisionists, as shown in [Figure 1].
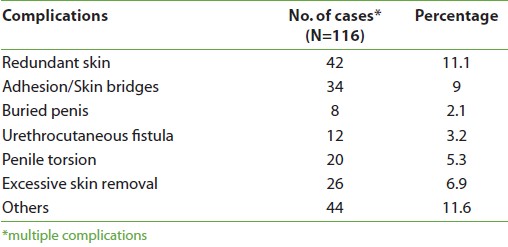
Post-circumcision complications were seen in 116 (33.7%) of circumcized children examined [Table 4].
The practice of circumcision is worldwide, with variation in the art and science peculiar to different localities. It is, probably, the most common procedure in the world, and has been practiced by Babylonians, Egyptians, and West African Negroes for over 5000 years. [11] This study showed that circumcision is an inherent part of life of people in Ilorin; hence, using mothers/parents of under-5 children gave a quick and reliable recall of the practice of circumcision and the events surrounding it. The prevalence of female circumcision among mothers was 65.6%. This prevalence rate is higher than what is generally quoted as an average, in Nigeria (25.1- 40%), [6] and 53.2% in a study by Ugboma et al. [12] in Omoku community in Egema-Ndoni LGA of Rivers State of Nigeria, though lower than the female circumcision prevalence report of more than 90% by Ebomoyi [13] in Ilorin and the survey report for Kwara. [6] This may reflect the effect of campaign against female genital mutilation (FGM), and possibly, also a false declaration of circumcision status by the respondents. Female circumcision is still being practiced in the community as reflected in the incidence rate of 73.9% among index female children examined during this study. This might be due to the strong influence of religion and cultural practices on the lifestyle of the people, since majority of them are Muslims. Study has shown that female circumcision is commoner among Muslims. [14] Many even believe that it makes delivery easier and assures safety of the newborn. [15],[16] Hence, female circumcision, in spite of public outcry against FGM/C, is still being practiced. [17] The circumcision rate was 87.5% among the under-5 is similar to the report by Okeke et al. [8] in Ibadan, though higher than the world average of between 25% and 33.3%. [18],[19] It is less than the rate in Israel, where virtually, every male is circumcized even as neonates. [20] Fewer neonatal circumcisions were done in this study, unlike what is practiced in the USA, [21],[22] Australia, [23],[24],[25] and Israel. [20] Neonatal circumcision was mainly done by doctors; other children were circumcized after the 40 th day of life, as a general customary practice. The high record of ‘doctors’ doing circumcision may not be unconnected with this false claim by male nurses and quacks owning private clinics that they are medical doctors and as assumed by the community. However, Ugboma’s [12] study showed that doctors were the highest operators of female genital mutilation for various reasons, though in this study, traditional circumcisionists did most of the female circumcision. Early circumcision by doctors and nurses, in this study, as against the delayed practice by the traditional circumcisionists, might have arisen because of the expertise involved and cultural practice. Many of the elite wanted the process concluded before resumption of duty after six weeks of maternity leave. The people of pacific origin prefer their children to be circumcized between the age of 6 and 10 years, [26] and it is reported that the Xhosa tribe in Eastern Cape, South Africa, performs adolescence circumcision as an initiation rite to manhood. [27] This study showed that circumcision is done usually between one to three years of age in the local community. More circumcision occurred outside the hospital, and even at home, by the auxiliary nurses, community health extension workers, and traditional circumcisionists, who were not usually distinguished by the people from orthodox doctors and nurses. This is still lower than what is practiced in certain areas of the world. [20],[27] Culture dominated reasons for circumcision among respondents in spite of the fact that majority of respondents were Muslims, and male circumcision is prescribed by the religion. This agreed with the facts that it is done for initiation to manhood as cultural cutting predates Islam. Traditional opening of foreskin excision with the application of local preparations, such as herbal based paste and black soap, to control bleeding and aid healing, still predominate, and orthodox medical techniques are being practiced only in the hospitals. The use of Plastibel TM (ring-type) for circumcision is practiced mainly by doctors and occurred in about a third of all circumcised male children in this study; this is in concordance with a survey by Popoola et al. [28] in Ilorin. The use of Gomco TM is still low in this study and in the review by Popoola. [28] Bleeding and delayed wound healing were experienced in the early post circumcision period and was commonest among the children that were circumcized by traditional circumcisionists. Early complication rates have reported to range up to 55%. [29],[30] Post circumcision bleeding could be life threatening and many of these children might have earned unscheduled admission in hospitals because of the need of blood transfusion, whereas others might have ex-sanguinated to death. [31] We lack appropriate report of events in our environment, and incidence of death from circumcision might have been taken as an ‘act of God’. Complications are known to follow any surgical procedure, and circumcision is not excluded, though the world average for circumcision ranged between 0.19% and 3.1%, when some ‘minor’ complications were excluded, [20],[32],[33] this study revealed a rate of 30.1% which is unacceptable and even higher than the 20% reported by Okeke. [8] The high redundant skin complication rate is in agreement with the findings of Ben Chaim et al. [20] in Israel and Yegane et al. [34] in Iran. The skin bridges arose from redundant skin adhesion, ragged and infection of wound. [35],[36],[37] For generations to come, circumcision would be practiced as dictated by religion and culture, and if the campaign for its use to reduce the incidence of HIV infection succeeds, then more would be done and possibly at early ages. To reduce the high complication rate, proper enlightenment and retraining of health care providers and traditional circumcisionists must be done. This should emphasize the safe methods available, and how to use them. Mothers or all women in the reproductive age group should be counseled about circumcision, and what to expect following male circumcision. The government should involve the religious leaders and influential personalities in the community for the prevention of negative and harmful traditional practices including female circumcision.
The authors wish to thank the Head of Department of Epidemiology and Community health of University of Ilorin, the Community leaders in the study area, and the research assistants for their support in making this project a success.
Source of Support: None, Conflict of Interest: None
[Table 1], [Table 2], [Table 3], [Table 4] |
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||