| Abstract |
Aims and Objective : To ascertain the cytological diagnosis of metastatic lesions with special reference to clinicopathological analysis of primary site in cases of epithelial tumors. Materials and Methods: One hundred and seventy-one suspected metastatic lesions were aspirated with a 22-23-G needle and smears were fixed and stained. The cases in which the primary site was not evident at the time of initial presentation were subsequently subjected to thorough physical examination followed by radiological investigations for the search of the primary site. Histopathological examination was performed in 16 cases with inconclusive cytological impression. Results: Of the total 171 cases of metastatic lesions, 155 (90.6%) were diagnosed by fine needle aspiration biopsy and 16 (9.4%) were diagnosed by histopathology. Majority of the cases [81 (47.4%)] were observed in the fifth decade of life, followed by 76 cases (44.4%) in the sixth decade and 11 cases (6.4%) in the seventh decade of life. Lymph nodes were the most frequent site of metastasis [115 cases (67.3%)], with a majority in the cervical group. The oropharynx including the oral cavity and pharyngolarynx was observed to be the most common primary site in 55 cases (32.2%). Conclusion: An accurate pathologic assessment of the malignant tissues in conjunction with pertinent clinical data helps in the evaluation of metastatic cases.
Keywords: Fine needle aspiration biopsy, metastatic tumor, primary tumor
| How to cite this article: Ahmad S, Akhtar K, Singh S, Siddiqui S. Fine needle aspiration biopsy of metastatic lesions with special reference to clinicopathological analysis of primary site in cases of epithelial tumors. Ann Trop Med Public Health 2011;4:7-11 |
| How to cite this URL: Ahmad S, Akhtar K, Singh S, Siddiqui S. Fine needle aspiration biopsy of metastatic lesions with special reference to clinicopathological analysis of primary site in cases of epithelial tumors. Ann Trop Med Public Health [serial online] 2011 [cited 2020 Aug 9];4:7-11. Available from: https://www.atmph.org/text.asp?2011/4/1/7/80514 |
| Introduction |
The dilemma associated with the diagnosis of metastatic lesion with no obvious primary site has long been a challenge for the clinicians.
The detection of metastases constitutes decisive evidence for categorizing a proliferating primary lesion. Fine needle aspiration biopsy (FNAB) helps in confirming a clinical suspicion of local recurrence or metastasis of known cancer without subjecting the patient to further surgical intervention. [1]
The present study was undertaken to ascertain the cytological diagnosis of metastatic lesions with special reference to clinicopathological analysis of primary site in cases of epithelial tumors.
| Materials and Methods |
The present study was conducted on 171 cases of metastatic malignancy, attending the Inpatient and Outpatient Departments of Radiotherapy and Pathology of J.N. Medical College, A.M.U., Aligarh.
All the cases underwent a basic evaluation consisting of history, physical examination (including careful breast palpation and pelvic examinations in women and testicular and prostate examinations in men), laboratory studies (including liver function tests and hemogram), chest radiography, computed tomographic scans of the abdomen and pelvis and mammography in women. When indicated by positive findings during this initial evaluation, additional diagnostic tests were performed. These selective tests included sputum cytology, computerized tomography (CT) scan of the chest and gastrointestinal endoscopy. All suspected metastatic lesions were subjected to fine needle aspiration with a 22-23-G needle, and whenever necessary, under ultrasound and CT guidance. Smears were fixed in 95% alcohol and stained by Hematoxylin and Eosin (H and E) and Papanicolaou stains.
Histopathological examination was performed in 16 cases with inconclusive cytological impression after paraffin embedding and staining with H and E stain.
| Results |
Majority of the cases [81 (47.4%)] were observed in the fifth decade of life, followed by 76 cases (44.4%) in the sixth decade and 11 cases (6.4%) in the seventh decade of life. However, three cases were seen in the age group of 0-20 years, with a case of a 14-year-old girl with pleural and peritoneal effusions and diagnosed metastatic juvenile granulosa cell tumor of the ovary. Another case of metastatic Wilm’s tumor in a 3-year-old boy presenting with subcutaneous scalp swelling was observed by us. Fifty-seven percent of cases were men and 43% were women.
Observing the distribution of cases according to metastatic sites, lymph nodes were the most frequent site in 115 cases (67.3%), followed by bone in 17 cases (9.9%), liver in 15 cases (8.8%) and skin metastasis in 14 cases (8.2%) [Table 1]. Among the lymph nodes, cervical group accounted for 65 cases (56.5%), followed by 31 cases (27.1%) of axillary nodes.
| Table 1: Primary tumor sites and their respective metastatic sites
Click here to view |
The oropharynx including the oral cavity and pharyngolarynx was the most common primary site observed in 55 cases (32.2%), followed by a primary breast tumor in 38 cases (22.2%) with 31 cases (81.6%) metastasizing to axillary nodes. Primary in the gastrointestinal tract comprised 20 cases (11.7%), 14 cases (8.2%) had primary in the lungs and there were 8 cases (4.7%) each of primary tumor in female and male genital tracts. A total of 15 cases (8.8%) studied by cyto-histopathology presented as metastatic cancer of unknown primary site [Table 2].
| Table 2: Distribution of cases according to primary site
Click here to view |
In the cervical group of nodes, the predominant cytological diagnosis was squamous cell carcinoma [56 cases (86.2%)] with smears showing cohesive sheet of tumor cells with high N/C ratio and nuclear hyperchromasia [Figure 1], followed by adenocarcinoma in 5 cases (7.7%) and anaplastic carcinoma in 4 cases (6.1%).
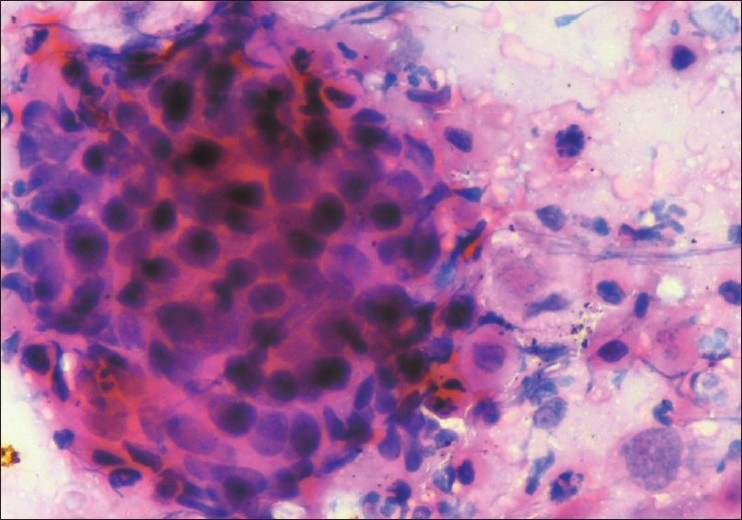 |
Figure 1: Poorly differentiated squamous cell carcinoma: Smear shows cohesive sheet of tumor cells with high N/C ratio and nuclear hyperchromasia (H and E, ×400)
Click here to view |
The axillary group was found to be the most important site of metastatic breast carcinoma [31 cases (100%)].
In the supraclavicular lymph nodes, there were 4 cases (57.1%) of metastatic adenocarcinoma, 2 cases (28.6%) of metastatic squamous cell carcinoma and one case (14.3%) of metastatic ductal carcinoma breast.
The inguinal group of lymph nodes formed an important metastatic site from the male external genitalia and ovaries. The predominant cytological diagnosis was adenocarcinoma in 3 cases (50%), and 2 cases (33.3%) of metastatic malignant melanoma, with smear showing pleomorphic tumor cells with enlarged eccentric nuclei and eosinophilic granular cytoplasm and a single case (16.7%) of undifferentiated carcinoma.
In the bone, 9 cases (52.9%) were diagnosed on FNAB as metastatic adenocarcinomas. Almost all cases with skeletal metastases showed metastatic foci in the vertebral column and the upper end of femur, while there was a single case of metastatic foci at the upper end of humerus in a case of breast carcinoma.
In the liver, 11 cases (84.6%) were found to be of metastatic adenocarcinoma on cytological examination with majority of the primary lesions located in the gall bladder and gastrointestinal tract.
Skin showed 3 cases (21.4%) of metastatic adenocarcinoma; all of which had primaries in the lung. A single case of squamous cell carcinoma lung with metastasis to skin was also seen. Most of the metastatic tumors were located on the anterior chest wall, [8 cases (57.1%)], followed by nodules on the scalp [5 cases (35.7%)] and a single case was located on the skin around the elbow.
Histopathological examination of suspected primary site was performed in 16 cases and also in the same number of cases where cytology of metastatic site was inconclusive, either due to hemorrhagic and necrotic background or poor representative cellularity. Mesenteric lymph node was observed as a metastatic site in three cases with primary being adenocarcinoma intestine. There were five cases of metastatic bone tumors and two cases of metastatic papillary adenocarcinoma of liver with primary colorectal tumor. Omentum was observed as a site of metastasis in four cases (25%) with primary site being the ovaries in all the cases. Two cases were observed to be ovarian cystadenocarcinoma with peritoneal implants and one case each of granulosa cell tumor and yolk sac tumor of ovary with peritoneal implants were seen.
An isolated case of endometrial choriocarcinoma with metastasis to the central nervous system was noted where contrast-enhanced computed tomography (CECT) head showed multiple nodular and ring enhancing lesions in bilateral cerebral hemisphere with surrounding edema [Figure 2] along with a case of adenosquamous carcinoma of the cervix with extension into the uterine cavity. All the primary tumor sites with respective metastatic sites are depicted in [Table 2].
| Figure 2: Contrast-enhanced computed tomography (head) shows multiple nodular and ring enhancing lesions in bilateral cerebral hemisphere with surrounding edema secondary to choriocarcinoma
Click here to view |
| Discussion |
Patients with a suspected metastatic lesion were included in the present study and evaluated by means of a careful history, physical examination, pathologic review and axillary radiological investigations to ascertain the primary site.
Majority of the lesions, i.e., 90.6% were diagnosed by FNAB, a modality of immense help as it is rapid, safe and cost-effective in determining the nature of a variety of metastatic lesions.
Our study revealed a slight male predominance with more than 85% cases between 40 and 60 years and above, which corresponds to the series reported by Didolkar et al. [2] The youngest patient was a 3-year-old boy with a subcutaneous scalp swelling, who was found to be harboring a metastatic Wilm’s tumor.
On analysis of frequency of metastatic tumors at various metastatic sites, we observed that lymph nodes were the most common sites (67.3%), an observation in concordance with the findings of 76.8% by Sinha et al. [3] Snee and Vyramuthu [4] observed bone to be the most frequent site of metastasis (55.0%) followed by lymph nodes in 28% cases.
The second most frequent site in our study was the bone (9.9%) followed by the liver (8.8%). Similarly, Sinha et al. [3] also observed bone to be the second most frequent metastatic site (9.6%) followed by liver (7.7%).
The distribution of primary tumors at various metastatic sites in our study showed pharyngolarynx and oral cavity to be harboring the maximum number of cases (32.2%). Sinha et al. [3] also observed maximum number of primaries in pharyngolarynx and oral cavity. However, our findings are not in accordance with those of Didolkar et al. [2] who reported lung (40%) to be the most common primary site, followed by pancreas and stomach (6.5% each).
In our study on analysis of cytohistological diagnosis of metastatic lesions, we observed squamous cell carcinoma to be the predominant type of tumor (38.2%), followed by adenocarcinoma in 26.8% cases. Similar findings have been reported in studies by Sinha et al. [3] But our observations differed from those made by Didolkar et al. [2] who reported metastatic adenocarcinoma as the most common type of tumor (61% cases). This discrepancy could be because these authors restricted their study strictly to metastatic lesions with unknown or occult primary and excluded all cases with a known primary detected through history, clinical examination and radiological work up.
Cervical nodes were the commonest metastatic site, with squamous cell carcinoma being the commonest cytomorphological type in our study, a finding similar to that reported by Sinha et al. [3] and Jacobson et al. [5]
Thirty-one cases had metastatic lesions in the axillary group of lymph nodes, all of which had a primary in the breast. Similar findings were also observed by Sinha et al. [3] and Copeland et al. [6] Carter et al. [7] asserted that tumor size and extent of axillary lymph node involvement were found to act as important independent but additive prognostic indicators in cases of breast cancer.
Metastatic lesion in supraclavicular lymph nodes was observed in seven cases; with lung being the most common primary site, three cases (42.9%) followed by two cases (28.6%) of metastasis from the colorectum and a single case each from breast and an unknown primary. Similar observations were also made by Sinha et al. [3] who observed lung to be an important primary site for metastasis in the right supraclavicular lymph nodes.
Our study included six cases of metastases to inguinal lymph nodes. Three cases (50%) had a primary in male genital tract and two cases (33.3%) were metastatic malignant melanoma, while there was a single case of undifferentiated carcinoma. Copeland et al. [6] also observed malignant lesions arising in the lower extremity, perineum, male and female genital tracts to be important primary sites for inguinal lymph node metastases.
We observed prostate in males (23.5%) and breast in females (17.6%) to be the most common primary sites with skeletal metastasis. Our findings are concordant with the observation of Hage et al. [8] who observed primary tumors in prostate and breast in 31.2 and 30.6% cases, respectively. Katagiri et al. [9] observed lung to be the most frequent primary site (35.5%), followed by prostate (17.2%) and breast (7.8%). Buckwalter [10] in his autopsy studies has revealed that 50-70% of prostatic cancer patients developed skeletal metastasis during the course of their disease.
The most common sites of primary tumors with hepatic metastases in the present study were gall bladder and colorectum in 33.3 and 26.7% cases, respectively, with 86.7% metastatic lesions being adenocarcinoma. This observation is in agreement with the findings of Ayoub et al. [11] in their studies on liver metastasis.
Our study revealed anterior chest wall (57.1%) and scalp (35.7%) to be the most common site of metastases in the skin. Similar findings have been reported by Brownstein and Hellwig, [12] who observed anterior chest wall and head and neck to be the most common site for metastasis in the skin. Saikia et al. [13] have stated that the skin on the entire body, and especially the scalp, should be examined carefully when a primary internal malignancy or recurrence of one is suspected.
| Conclusion |
The most critical aspect of the evaluation of metastatic cases is the accurate pathologic assessment of the malignant tissues in conjunction with pertinent clinical data. Such close collaboration between the clinician and the pathologist may maximize the diagnostic potential in treatable primary tumors.
| References |
| 1. | Christopherson WM. Cytologic detection and diagnosis of cancer: Its contributions and limitations. Cancer 1983;51:1201-8. |
| 2. | Didolkar MS, Fanous N, Elias EG, More RH. Metastatic carcinomas from occult primary tumours. Ann Surg 1977;23:625-30. |
| 3. | Sinha SK, Basu K, Bhattacharya A, Banerjee U, Banerjee D. Aspiration cytodiagnosis of metastatic lesions with special reference to primary sites. Journal of Cytology, 2003;20:16-8. |
| 4. | Snee MP, Vyramuthu N. Metastatic carcinoma from unknown primary site: The experience of a large oncology center. British J of Radiology, 1985;58:1091-5. |
| 5. | Jakobson PA, Engzell U, Sigurdson A, Zajicek J. Aspiration biopsy of metastatic carcinoma in lymph nodes of the neck. Acta Otolaryn 1971;72:138-47. |
| 6. | Copeland EM, McBride CM, Underwood RD. Axillary metastases from unknown primary sites. Ann Surg 1973;178:25-7. |
| 7. | Carter CL, Allen C, Henson DE. Relation of tumour size, lymph node status and survival in 24,740 breast cancer cases. Cancer 1989;63:181-7. |
| 8. | Hage WD, Aboulafia AJ, Aboulafia DM. Incidence, location and diagnostic evaluation of metastatic bone disease. Orthop Clin of North Am 2000;31:515-28. |
| 9. | Katagiri H, Takahashi M, Inagaki J, Sugiura H, Ito Shigeki, Iwata H. Determining the site of primary cancer in patients with skeletal metastasis of unknown origin. Cancer 1999;86:533-7. |
| 10. | Buckwalter JA. Metastatic disease of the skeleton. Am Fam Physician 1997;55:1761-8. |
| 11. | Ayoub JP, Hess KR, Abbruzzese MC, Lenzi R, Raber MN, Abbruzzese JL. Unknown primary tumours, metastatic to liver. J Clin Oncol 1998;16:2105-12. |
| 12. | Brownstein MH, Helwig EB. Patterns of cutaneous metastasis. Arch Derm 1972;105:862-8. |
| 13. | Saikia B, Dey P, Saika UN, Das A. Fine aspiration cytology of metastatic scalp nodules. Acta Cytologica 2001;45:537-41. |
Source of Support: None, Conflict of Interest: None
| Check |
DOI: 10.4103/1755-6783.80514
| Figures |
[Figure 1], [Figure 2]
| Tables |
[Table 1], [Table 2]



