| Abstract |
Tuberculosis of the liver is rare and is generally seen as a part of disseminated tuberculosis. With the advent of HIV, isolated tuberculous involvement of the liver has been seen. Here we report a case of isolated tuberculous liver abscess in an immunocompetent patient.
Keywords: Immunocompetent liver, liver abscess, tuberculosis liver
| How to cite this article: Shetty JB, Prabhu V L, Joshi AS, Kulkarni DV. Isolated tuberculous liver abscess in an immunocompetent patient. Ann Trop Med Public Health 2012;5:137-8 |
| How to cite this URL: Shetty JB, Prabhu V L, Joshi AS, Kulkarni DV. Isolated tuberculous liver abscess in an immunocompetent patient. Ann Trop Med Public Health [serial online] 2012 [cited 2021 Mar 6];5:137-8. Available from: https://www.atmph.org/text.asp?2012/5/2/137/95974 |
| Introduction |
Involvement of the liver in miliary tuberculosis is well-known and accounts for 50-80% of all cases dying from pulmonary tuberculosis. However, isolated tuberculosis of the liver presenting as an abscess is very rare. Less than 25 cases have been documented in the imaging literature to date. [1] With the advent of HIV, bizarre presentations of tuberculosis are encountered including involvement of the liver. Here we report a rare case of isolated tuberculous abscess of the liver in an immunocompetent patient. The clinical findings are non-specific and even latest diagnostic modalities like ultrasound and computed tomography can miss the diagnosis. Awareness of this rare clinical entity may prevent needless surgical intervention.
| Case Report |
A 60-year-old female patient was admitted with history of pain in the right hypochondrium since one month and nausea and vomiting since three to four days. She also complained of loss of appetite since one month.
On examination she did not have icterus, lymphadenopathy or pedal edema. On abdominal examination there was tenderness in the epigastrium and right hypochondrium. The liver was enlarged (eight cm below the right costal margin). The surface was smooth and a diffuse swelling was palpable in the epigastrium.
Hematological investigations revealed a serum hemoglobin level of 11.8 g% and total leucocyte count of 9,700 per cumm. Erythrocyte sedimentation rate was 48 mm at the end of one hour. Liver function tests showed slightly raised aspartate aminotransferase SGOT) and alanine aminotransferase (SGPT). Chest X-ray did not reveal any abnormality.
Ultrasonography of the abdomen showed left liver lobe abscess measuring approximately 11 × 7 cm. Right lobe of the liver was normal. Ultrasonography (USG)-guided aspiration of the abscess was done and the material was sent for culture. Culture sensitivity and Gram staining revealed no growth and organisms respectively. Unfortunately, it was not cultured for tuberculosis. Patient was taken for laparotomy and lateral segmentectomy was done.
We received the specimen for histopathological examination. On gross examination there was an abscess cavity measuring 11 x 9 x 6 cm. The cavity was covered with exudative material. Histopathological examination of the tissue showed many epithelioid cell granulomas [Figure 1] and [Figure 2] with foci of caseation necrosis [Figure 3]. Ziehl-Neelsen staining of the tissue revealed acid-fast bacilli (AFB). Based on the above findings a diagnosis of tuberculous abscess was given. Patient was started on antituberculous treatment (ATT) and she responded favorably.
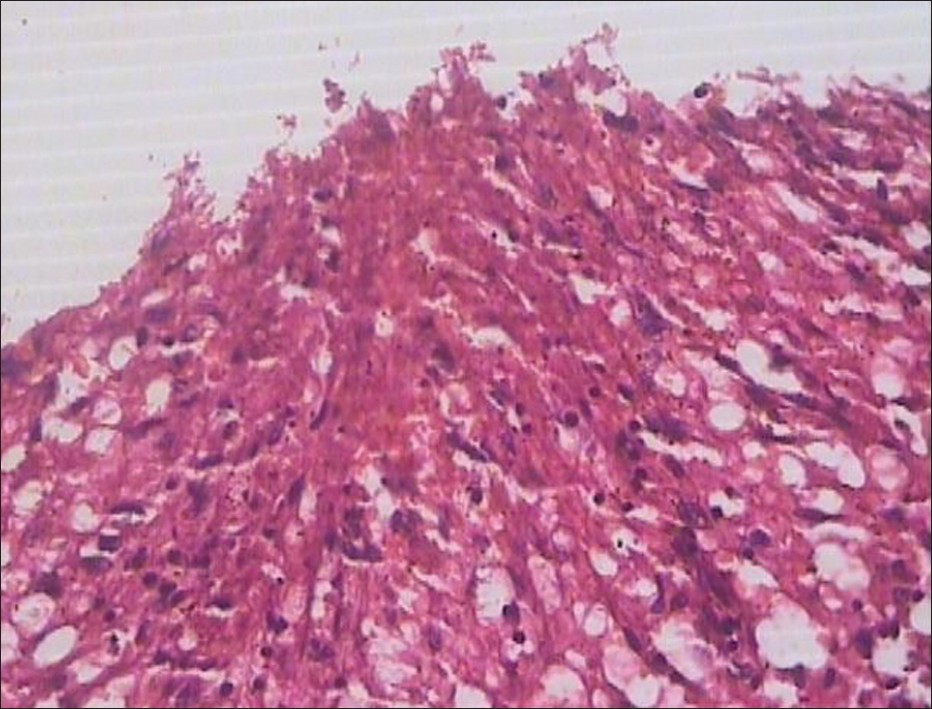 |
Figure 1: Section from liver abscess showing aggregation of epithelioid cells (H and E, ×400)
Click here to view |
| Figure 2: Section from liver abscess showing foci of caseation necrosis (H and E, ×400)
Click here to view |
| Figure 3: Section from liver abscess showing epithelioid cell granuloma (H and E, ×400)
Click here to view |
| Discussion |
Hepatic tuberculosis is usually associated with an active pulmonary or miliary tuberculosis but rarely localizes as a liver mass. [2] Tubercle bacilli reach the liver by hematogenous dissemination, the portal of entry in case of hepatic miliary tuberculosis is through the hepatic artery whereas in case of focal liver tuberculosis it is through the portal vein. [3] The rarity of the focal form of hepatic tuberculosis may be because the liver is resistant to challenge with tubercle bacilli due to the relatively low tissue oxygen tension. [4] Bestowe was the first to describe tuberculous liver abscess in 1858. [5] Hepatic involvement with Mycobacterium tuberculosis has been reported in 7.5% of patients with HIV infection and tuberculosis. [6] Here in the present case the patient was immunocompetent and also there was no evidence of focus of tuberculosis elsewhere in the body.
Tuberculous liver abscess must not be confused for hepatoma or pyogenic liver abscess. [2] Presence of caseating granulomatous lesions in the biopsy and or presence of AFB in such material is the hallmark of diagnosis. [7] AFB are rarely demonstrated in liver tuberculosis. The presence of AFB although highly suggestive of tuberculosis cannot be relied on with certainty as atypical mycobacteriosis is an increasing cause of hepatic granuloma, especially with the advent of AIDS. [8] The absence of AFB should not detract from diagnosis, particularly in endemic areas of tuberculosis. [2]
Thus, to conclude, any liver abscess should be evaluated for tuberculosis as the prognosis of this entity is excellent with appropriate ATT, and also it will prevent unnecessary surgical intervention.
| References |
| 1. | Chen HC, Chao YC, Shyu RY, Hsieh TY. Isolated tuberculous liver abscesses with multiple hyperechoic masses on ultrasound: A case report and review of the literature. Liver International 2003;23:346-50. |
| 2. | Bangroo AK, Malhotra AS. Isolated hepatic tuberculosis. J Indian Assoc Pediatr Surg 2005;10:105-7. |
| 3. | Javid G, Khan BA, Shah AH, Khan MA. Isolated tuberculous liver abscess. J Assoc Physicians India 1998;46:973-4. |
| 4. | Nand N, Aggarwal HK, Singh M, Dayanand. Tuberculous liver abscess. J Assoc Physicians India 2000;48:244-6. |
| 5. | Stevens A, Little JM. Isolated tuberculous hepatic abscess. Aust N Z J Surg 1987;57:409-11. |
| 6. | Amarapurkar DN, Chopra KB, Phadke AY, Sahni S, Prabhu SR, Kalro RH. Tuberculous abscess of the liver associated with HIV infection. Indian J Gastroenterol 1995;14:21-2. |
| 7. | Roy R, Goyal RK, Gupta N. Tuberculous liver abscess. J Assoc Physicians India 2000;48:241-3. |
| 8. | Vishwanathan R, Jain S, Pandey MB, Shah A, Vishwanathan I. Hepatic abscess due tuberculosis in an immunocompetent patient. Bombay Hosp J 2004;46:313-4. |
Source of Support: None, Conflict of Interest: None
| Check |
DOI: 10.4103/1755-6783.95974
| Figures |
[Figure 1], [Figure 2], [Figure 3]



