| Abstract |
Three cases of rhinocerebral mucormycosis (RCM) with different courses of illness following a common standardized treatment protocol are discussed. Seen predominantly in diabetics. Clinical picture is often blurred by overlapping features of chronic rhinosinusitis. CT picture is helpful in assessing extent. Histopathological evidence is diagnostic. We describe three cases of RCM with different presentations but followed same treatment protocol. RCM is not just a disease of chronic uncontrolled diabetics. Its indolent clinical course doesn’t correlate with its aggressive pathology for which strict treatment protocol to be followed. In suspected cases of RCM, improvement of predisposing diseases, radical surgical debridement and effective systemic antifungal therapy must be instituted immediately. Absence of intracranial or orbital extension are indicators of good prognosis. Ketoacidosis is the single most important detrimental factor.
Keywords: Amphotericin-B, diabetic ketoacidosis, rhinocerebral mucormycosis
| How to cite this article: Vaidyanathan V, Shetty K. Rhinocerebral mucormycosis: A series of 3 cases. Ann Trop Med Public Health 2012;5:591-3 |
| How to cite this URL: Vaidyanathan V, Shetty K. Rhinocerebral mucormycosis: A series of 3 cases. Ann Trop Med Public Health [serial online] 2012 [cited 2013 Jul 5];5:591-3. Available from: https://www.atmph.org/text.asp?2012/5/6/591/109291 |
| Introduction |
RCM is also known as phacomycosis or zygomycosis, is a rare fatal opportunistic in fection caused by the family of mucoraceae (Mucor, Rhizomucor, Rhizopus, Absidia species) that are commonly found in soil and among decaying vegetation. [1],[2] RCM is usually seen in diabetics, especially in ketoacidosis, but may also appear in healthy people. [3] Several clinical forms are described such as rhino-orbital-cerebral, pulmonary, disseminated, cutaneous, and gastrointestinal. Rhino-orbital-cerebral is the most common form in diabetic patients. [4] Initially majority of patients complain about the typical symptoms of acute bacterial rhinosinusitis but they deteriorate rapidly and do not respond to conventional treatment, such patients are usually associated with diabetic ketoacidosis (DKA). Early CT imaging is usually unimpressive. Direct extension and dissemination via blood leads to orbital and intracranial complications. [1] The diagnosis is confirmed histologically and culture is used to identify the specific species. The treatment of mucormycosis includes aggressive surgical debridement and systemic antifungal therapy. Early diagnosis and prompt initiation of treatment is essential for a successful outcome. Disease extending beyond the sinus mucosa and associated DKA on initial presentation are poor prognostic indicators. [5] Newer drugs like Posaconazole and micafungin are being tried with Amphotericin B with variable results. Three cases of RCM are discussed which had a variable clinical course following standard treatment protocol.
| Case Reports |
Case 1
50 yrs old male, chronic diabetic presented with c/o intermittent fever with pus discharging from the right nasal cavity and oral cavity through an oroantral fistula. This was associated with swelling of the right lower eyelid and cheek since one week. His vision and eye movements were normal. CT scan-uniform homogenous opacity filling right maxillary sinus with premaxillary soft tissue oedema and fistulous defect in the alveolar arch of maxilla [Figure 1]. Fungal studies suggestive of mucormycosis. He was admitted and blood sugars were controlled aggressively by concomitant administration of amphotericin B and endoscopic debridement showed extensive damage to the lateral nasal wall. The patient remains disease free on successive follow up.
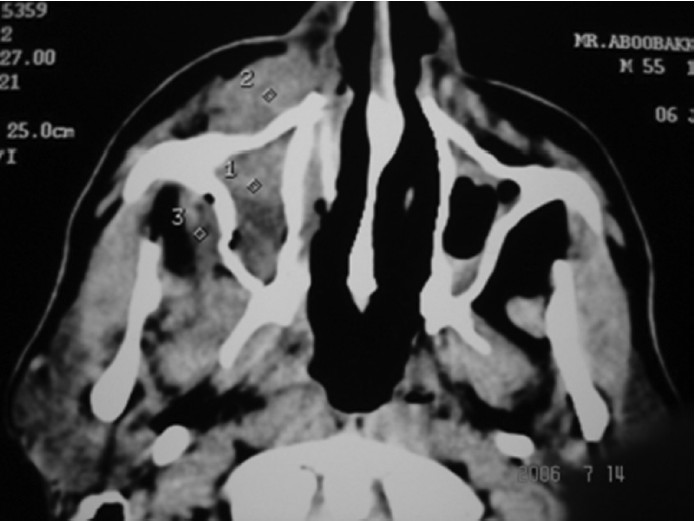 |
Figure 1: Homogenous opacification of right maxillary sinus peri maxillary soft tissue infiltration
Click here to view |
Case 2
34 yrs male, non diabetic presented with c/o unilateral headache. O/e he had loss of sensation over left cheek. CT scan – isolated b/l sphenoid sinus disease with no intracranial extension or bony defect [Figure 2]. He underwent endoscopic surgery, pus and grannulation in sphenoid sinus revealed mucormycosis. He received both plain and liposomal amphotericin B. He later developed TB meningitis with obstructive hydrocephalus. There have been no proven recurrences but the patient continues to have a high morbid state.
| Figure 2: (a) Isolated sphenoid disease with no intracranial extension. On MRI T2 weighted image there are no features of CVT, (b) Isolated sphenoid disease with no intracranial extension. On MRI T2 weighted image there are no features of CVT
Click here to view |
Case 3
50 yrs male, newly detected diabetic. H/o endoscopic surgery and i.v. amphotericin B-1 gm 2 months back for right maxillary sinus mucormycosis. Now c/o right sided blood stained nasal discharge and diffuse facial swelling extending upto zygoma with loss of sensation over right cheek. CT scan – mucosal thickening in the right maxillary sinus, no bony erosion, no evidence of disease [Figure 3]. On endoscopy suspicious lesion biopsied on the medial maxillary wall which revealed recurrence of mucormycosis. He was treated with medial maxillectomy and amphotericin B. He has had various lifestyle modifications but remains disease free so far.
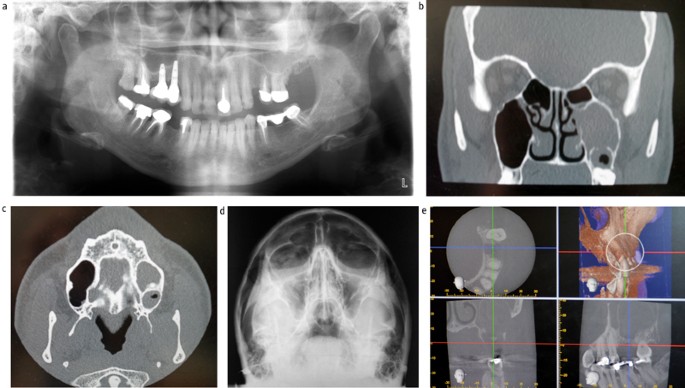 |
Figure 3: Mucosal thickening seen in maxillary antrum. A wide antrostomy can also be seen from previous surgery
Click here to view |
| Discussion |
Baker introduced the term ”rhinocerebral mucormycosis” as a malignant form of cephalic mucormycosis with a high mortality rate. In 1958 Chick et al, demonstrated the effectiveness of amphotericin B. Today, the most commonly chosen therapy consists of the treatment of predisposing diseases, radical surgery, and systemic antifungal medication, especially with amphotericin B. Despite these aggressive therapeutic measures the mortality continues to be very high. [1]
Mucormycosis in humans is usually initiated by inhalation of spores. When the fungi are introduced into nares of patients with serious underlying pathologic disorder, they induce a fulminant infection. [3]
Mucormycosis primarily causes tissue and blood vessel invasion.
Secondary effects are the development of thrombosis, hemorrhage and tissue necrosis causing local destruction of the affected organs. In addition, the resulting hypoxic environment promotes fungal proliferation. [1]
The most important predisposing factors are haematological disorders and poorly controlled diabetes mellitus, particularly if associated with DKA. Acidosis inhibits iron binding of transferrin, resulting in an increased proportion of unbound iron, which may promote the growth of the fungus or may also be due to decreased neutrophil chemotaxis and phagocytosis. [1],[4] Jung et al, In their case series reported 100% mortality with DKA hence proving to be the single most important detrimental factor. [6] Two of our patients were diabetic but neither one of them had ketoacidosis nor none had any other haematological disorder which might explain their low mortality.
The disease often presents with typical signs and symptoms of bacterial rhinosinusitis such as headache, fever, periocular pain, and facial swelling. It can rapidly progress to involve the surrounding tissue like the orbit, optic nerve and even the brain. Black eschar and necrotic debris in the nasal cavity are the usual endoscopic findings. [1],[6]
Initial CT imaging is generally not impressive and shows nonspecific, sinus mucoperiostal thickening or fluid collection. In all our cases the mucormycosis started showing only these unspecific symptoms. Perisinusal soft tissue infiltration may be an early CT finding in patients with rhinocerebral mucormycosis. [7]
In 80% of the patients, necrotic lesions of the nasal mucosa occur and can be seen as black eschar during the course of disease. [6] Diagnosis of rhinocerebral mucormycosis cannot be excluded even if there is a negative imaging study. The diagnostic confirmation is the histopathological report, which demonstrates angioinvasion by the irregular broad non-septated hyphae that branch at right angles. [8]
The treatment of mucormycosis traditionally consists of prompt administration of medical and surgical procedures. [6] Renal toxicity is common with amphotericin-B therapy hence new formulations would be less nephrotoxic such as LAT-B (liposomal amphotericin-B), amphotericin-B colloidal dispersion or lipid complex. [5] LAT-B tolerance is excellent and results only a minor increase in the serum creatinine level during the period of therapy. [6] Most of our patients who had renal toxicity were promptly changed to LAT-B. A surgical procedure is an important adjunct to the medical treatment regimen as it is difficult for the antifungal agent to reach and penetrate ischemic tissue. [1] Therefore, debridement has been recommended at frequent intervals. [1],[2],[3],[4],[5],[6],[7] LAT-B irrigation and nasal and orbital packing may be a reasonable modality for rhino-orbital mucormycosis. [2] We applied LAT-B via both systemically and locally in one of our cases which had an isolated sphenoid disease but, unfortunately he developed other complications. [4] Amphotericin-B can be used alone or in new combination therapy with other echinocandin such as micafungin which was successfully used by Ogawa et al. [5]
| Conclusion |
Treatment of suspected cases of RCM should include prompt initiation of improvement of predisposing diseases, radical surgical debridement and effective systemic antifungal therapy. Absences of intracranial or orbital extension are indicators of good prognosis. Diabetic ketoacidosis at presentation is the single most important detrimental factor. The initial clinical picture might cloud the aggressive nature of the disease. However disease prognosis cannot be effectively ascertained.
| References |
| 1. | Scheckenbach K, Cornely O, Hoffmann TK, Engers R, Bier H, Chaker A, et al. Emerging therapeutic options in fulminant invasive rhinocerebral mucormycosis. Auris Nasus Larynx 2010;37:322-8. |
| 2. | Cheema SA, Amin F. Five cases of rhinocerebral mucormycosis. Br J Oral Maxillofac Surg 2007;45:161-2. |
| 3. | Rangel-Guerra RA, Martínez HR, Sáenz C, Bosques-Padilla F, Estrada-Bellmann I. Rhinocerebral and systemic mucormycosis. Clinical experience with 36 cases. J Neurolog Sci 1996;143:19-30. |
| 4. | Dökmetas HS, Canbay E, Yilmaz S, Elaldi N, Topalkara A, Oztoprak I, et al. Diabetic ketoacidosis and rhino-orbital mucormycosis. Diabetes Res Clin Pract 2002;57:139-42. |
| 5. | Ogawa T, Takezawa K, Tojima I, Shibayama M, Kouzaki H, Ishida M, et al. Successful treatment of rhino-orbital mucormycosis by a new combination therapy with liposomal amphotericin B and micafungin. Auris Nasus Larynx 2012;39:224-8. |
| 6. | Jung SH, Kim SW, Park CS, Song CE, Cho JH, Lee JH, et al. Rhinocerebral Mucormycosis: Consideration of prognostic factors and treatment modality. Auris Nasus Larynx 2009;36:274-9. |
| 7. | Silverman CS, Mancuso AA. Periantral soft-tissue infiltration and its relevance to the early detection of invasive fungal sinusitis: CT and MR findings. AJNR Am J Neuroradiol 1998;19:321-5. |
| 8. | Munir N, Jones NS. Rhinocerebral mucormycosis with orbital and Intracranial extension: A case report and review of optimum management. J Laryngol Otol 2007;121:192-5. |
DOI: 10.4103/1755-6783.109291
| Figures |
[Figure 1], [Figure 2], [Figure 3]



