| Abstract |
Tricuspid valve endocarditis in non-addicted patients without underlying cardiac disease is extremely rare. Therefore, its diagnosis often presents a clinical challenge. We report a case of a 24-year-old female who presented with bilateral lower lobe cavitary pneumonia. She remained febrile in spite of 5 days of intravenous antibiotic therapy. On subsequent investigations, she was found to have isolated tricuspid valve endocarditis caused by Staphylococcus aereus. She was not an intravenous drug abuser and there was no underlying cardiac disease. She responded well to medical therapy. We report this case because of rarity of tricuspid valve endocarditis is a non-addicted person with structurally normal heart and its atypical presentation with paucity of cardiac symptoms at initial stage.
Keywords: Cavitary pneumonia, infective endocarditis, non-addict, tricuspid valve
| How to cite this article: Das SK, Bairagya TD, Bhattacharaya S, Chottopadhaya BP. Staphylococcal tricuspid valve endocarditis in a non-addicted patient with structurally normal heart. Ann Trop Med Public Health 2012;5:139-41 |
| How to cite this URL: Das SK, Bairagya TD, Bhattacharaya S, Chottopadhaya BP. Staphylococcal tricuspid valve endocarditis in a non-addicted patient with structurally normal heart. Ann Trop Med Public Health [serial online] 2012 [cited 2021 Mar 4];5:139-41. Available from: https://www.atmph.org/text.asp?2012/5/2/139/95975 |
| Introduction |
Infective endocarditis designates microbial infection of the endothelial surface of the heart and great vessels. The hallmark of the infection is the formation of an adherent, bulky mass of thrombotic debris and organisms, called vegetation. Ninety-two percent involvement is in the left side and 8% is in the right side. [1] Isolated tricuspid (TV) endocarditis accounts for 5%-10% of cases of infective endocarditis (IE). [2] Predisposing factors are congenital heart disease, insertion of the central venous catheter, placement of a pace maker or implantable defibrillator, intravenous drug abuse, alcoholism, immunodeficiency, and genital sepsis. [3],[4] Staphylococcus aereus is the usual pathogen. TVIE is thought to be rare because the right-sided congenital heart diseases are rare and the tricuspid and pulmonary valves are not strained because of low pressure, and oxygen saturation is low. [2] TV endocarditis is rarely considered in differential diagnosis of a febrile patient who is not an intravenous drug abuser or has no predisposing heart disease. Moreover, delay in diagnosis is common due to atypical presentations such as predominant respiratory symptoms or paucity of cardiac manifestation in the early stage of the disease. [5] Here, we describe a case of TV endocarditis which occurred in a young female who was not addicted to intravenous drugs and had no underlying heart disease. She initially presented with cavitary pneumonia which failed to respond with antibiotics. She subsequently made a complete recovery with 6 weeks intravenous antibiotics.
| Case Report |
A 24-year female patient attended the chest outdoor of our hospital with high fever with chill and rigor and cough with mucopurulent expectoration for two weeks. She was a nonsmoker, nonalcoholic and was not an intravenous drug abuser. She had no past history of any congenital or rheumatic heart disease. On examination, she appeared pale with pulse rate 120 beats/min, respiratory rate 24/min, blood pressure 120/84 mmHg and oral temperature 101 °F. Examination of respiratory system revealed bilateral course crepitations at both bases. There was no sign of infection in skin, oral cavity, bones, and joints. Examination of other systems was within normal limits. Blood examination revealed hemoglobin 8.8 g/dl, total leukocyte count of 8.2 × 10 9 /l, neutrophils 62%, lymphocytes 26%, and ESR -102 mm in the first hour. Chest x-ray revealed bilateral lower zone infiltrates with multiple cavitations [Figure 1]. Blood biochemistry and urinalysis were normal. Sputum for gram stain and acid-fast bacilli stain were negative. HIV serology was nonreactive. She was put on intravenous ceftriaxone and azithromycin. However, she remained febrile despite 5 days of antibiotic. She also developed a new pan-systolic murmur at the left sternal edge. There was no classical clinical sign of tricuspid regurgitation. Trans-thoracic echocardiography revealed mild right ventricular dilatation, moderate tricuspid regurgitation, pulmonary arterial hypertension (pulmonary arterial pressure 55 mmHg), and a vegetation of 1.4 × 0.4 cm size in the tricuspid valve [Figure 2]. Blood cultures on two consecutive days grew S. aereus which was sensitive to cloxacillin, co-amoxiclav, gentamicin, cotrimoxazole, and clarithromycin.
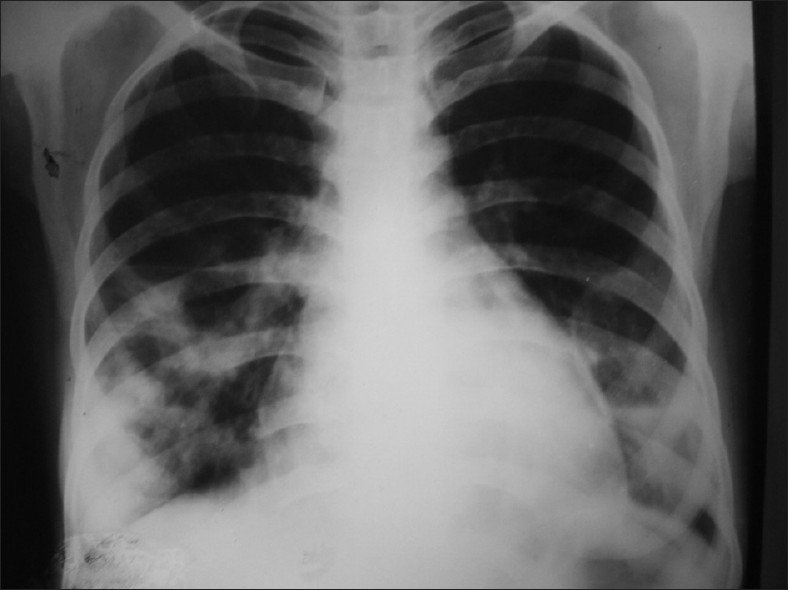 |
Figure 1: Chest X-ray (PA View) showing bilateral lower zone infiltrations with cavities.
Click here to view |
| Figure 2: Echocardiography showing vegetation in the tricuspid valve.
Click here to view |
A diagnosis of Staphylococcal endocarditis of TV was made on basis of Duke Criteria. She was treated with intravenous cloxacillin 2 g four times daily and gentamicin 80 mg IV thrice daily for six weeks. She made a complete recovery with normalization of chest radiograph, no residual vegetation in the TV, and sterile blood culture.
| Discussion |
Endocarditis of right heart valves is less common and almost always occurs in intravenous drug abusers, with more than 80% of TV endocarditis occurring in drug addicts. [6] Isolated TV endocarditis in patients with structurally normal heart who do not abuse intravenous drugs is unusual. Generally, it occurs in younger patients, [4] and the majorities have underlying medical conditions such as alcoholism, abortion, colonic disease, permanent catheter, and extra cardiac septic foci. [4],[5],[7],[8] Our case was a younger female but did not have any such abnormality.
The diagnosis is often delayed because the cardiac manifestation of the disease is subtle, and the murmur of tricuspid regurgitation is rarely present at initial presentation, [9] as occurred in our case. Persistent fever associated with pulmonary events, anemia, and microscopic hematuria, the so-called ”tricuspid syndrome,” are the signs of clinical alert for TV endocarditis. [7] Symptoms related to pulmonary septic emboli usually dominate the clinical picture and force the patients to seek medical advice. Pulmonary events may be of various forms including minor atelectesis, pulmonary infiltrate mainly in lower lobe with or without cavitations, and pleural effusion. Sometimes chest radiograph may be normal requiring CT Thorax to reveal the abnormality. Absence of peripheral stigma of infective endocarditis is the rule, rather than the exception. Sometimes joint, muscle, or skin may dominate the clinical picture making diagnosis more difficult. [8] Our case did not have hematuria or peripheral signs of infective endocarditis, but presented with persistent fever and cavitary pulmonary infiltrates.
As in any case is IE, Duke Criteria is the gold standard for diagnosis of native TVIE. Prognosis is excellent with intravenous bactericidal antibiotics which may need extension beyond six weeks. Only about 25% patient require surgery. [2],[10] Major indications of surgery are persistent sepsis despite appropriate antibiotic, recurrent pulmonary embolism and severe right heart failure. [11] Surgical options include vegetectomy and valvulectomy, valve repair, and valve replacement. [2],[3] Mortality is about 14%-24% which is lower than described for IE in patients with predisposing conditions. [11]
| References |
| 1. | Pachirat O, Chetchotisakd P, Klugboonkrong V, Tawelsangshuksakul P, Tantisivin C, Loapibon M. Infective endocarditis: Prevalence, characteristics and mortality in Khon Kaon, 1990-1999. J Med Assoc Thai 2002;85:1-10. |
| 2. | Chan P, Ogilby JD, Segal B. Tricuspid valve endocarditis. Am Heart J 1989;117:1140-6. |
| 3. | Morokuma H, Minato N, Kamohara K, Minematsu N. Three surgical cases of isolated tricuspid valve infective endocarditis. Ann Thorac Cardiovasc Surg 2010;16:134-8. |
| 4. | Naidoo DP. Right sided endocarditis in the non- drug addict. Postgrad Med J 1993;69:615-20. |
| 5. | Clifford CP, Eykyn SJ, Oakley CM. Staphylococcal Tricuspid valve endocarditis in patients structurally normal hearts and no evidence of narcotic abuse. Q J Med 1994;87:755-7. |
| 6. | Robbins MJ, Frater RW, Soeiro R, Frishman WH, Strom JA. Influence of vegetation size on clinical outcome of right sided infective endocarditis. Am J Med 1986;80:165-71. |
| 7. | Nandakumar R, Raju G. Isolated tricuspid valve endocarditis in non addicted patients: A diagnostic challenge. Am J Med Sci 1997;314:207-12. |
| 8. | Varona JF, Guerra JM. Tricuspid valve endocarditis in a non-addicted patient without predisposing myocardiopathy. Rev Esp Cardiol 2004;57:993-6. |
| 9. | Robins MJ, Soeiro R, Frishman WH, Strom JA. Right sided valvular endocarditis: Etiology, diagnosis and approach to therapy. Am Heart J 1989;111:128-35. |
| 10. | Roberts WC, Buchbinder NA. Right sided valvular endocarditis: A clinicopathological study of twelve necropsy patients. Am J Med 1972;5:7-19. |
| 11. | Rouviex E, Witchitz S, Bouvet E, Freidlander G, Wolff M, Regnier B, et al. Tricuspid infective endocarditis: 56 cases. Eur Heart J 1984;5:111-5. |
Source of Support: None, Conflict of Interest: None
| Check |
DOI: 10.4103/1755-6783.95975
| Figures |
[Figure 1], [Figure 2]



