| Abstract |
Background: Fever is usually associated with malaria parasitemia, and it is recommended that febrile children below the age of 5 years be treated with antimalarials. This study was undertaken to obtain information concerning the relationship between fever and the prevalence of malaria parasitemia among Nigerian children. Materials and Methods: Blood specimens from deep finger pricks of 730 children aged 0-2 years were examined for parasitemia using the Field’s stain method, and the axillary temperature of each subject was measured. Results: Malaria parasites were observed in 26.1% of the afebrile children and 40.6%, a statistically significant difference, in febrile children. Furthermore, 59.2% of the febrile subjects had no detectable malaria parasites in their blood. Conclusions: Fever is not always indicative of parasitemia, and subjects with asymptomatic infection must be regarded as a significant reservoir of transmissible malaria parasites within the study environment.
Keywords: Antimalarial, asymptomatic, children, fever, malaria, parasitemia
| How to cite this article: Onanuga A, Igbeneghu OA, Lamikanra A. A study of the relationship between the observation of fever symptoms and parasitemia among children in the Federal Capital Territory, Nigeria. Ann Trop Med Public Health 2015;8:1-4 |
| How to cite this URL: Onanuga A, Igbeneghu OA, Lamikanra A. A study of the relationship between the observation of fever symptoms and parasitemia among children in the Federal Capital Territory, Nigeria. Ann Trop Med Public Health [serial online] 2015 [cited 2020 Aug 15];8:1-4. Available from: https://www.atmph.org/text.asp?2015/8/1/1/156668 |
| Introduction |
Fever is an immune response capable of protecting the body from the effects of microbial infections. [1] In children, temperatures above 38°C measured rectally or 37.2°C measured under the arm are indicative of fever, which is frequently associated with infections. [2]
Annually, approximately 350-500 million cases of malaria kill up to three million people, with more than 90% of these deaths occurring in African children under 5 years of age. [3] It also accounts for 10-30% of all hospital admissions in malaria-endemic regions, especially Sub-Saharan Africa. [4]
Despite recent progress leading to the reduction of malaria morbidity and mortality, there are both empirical and theoretical evidence that the current suite of interventions is insufficient to eliminate malaria from those areas in Sub-Saharan Africa with high levels of malaria transmission. [5] In order to achieve reduced morbidity and mortality resulting from malaria, the infection must be recognized quickly so that patients are treated promptly. The clinical diagnosis of malaria is usually based on the patient’s symptoms, which include fever, chills, sweats, headaches, muscle pains, nausea, and vomiting, which are also associated with other diseases. This makes early diagnosis difficult, leading to delays in the commencement of treatment.
The World Health Organization (WHO) recommends that the treatment of malaria should be based on a laboratory-confirmed diagnosis, with the exception of children less than 5 years of age in areas of high transmission in whom treatment may be provided on the basis of a clinical diagnosis. However, the high prevalence of asymptomatic infections and lack of resources such as microscopes and trained microscopists in highly endemic areas have led peripheral health facilities to use “presumptive treatment.” Children who suffer from a fever that does not have any obvious cause are presumed to have malaria and are treated for that disease. Though this allows the rapid treatment of a potentially fatal disease, it can lead to incorrect diagnoses and unnecessary use of antimalarial drugs. [6] A study of the relationship between fever and the prevalence of Plasmodium falciparum parasitemia among children 0-2 years of age will give information that can serve as an important tool in the proper management of malaria among children in this age group and, more importantly, guide the judicious use of antimalarial drugs.
| Materials and Methods |
Study area
The study was carried out from April 1, 2008-March 31, 2009 in the Paediatric Out-patient Unit of the University of Abuja Teaching Hospital, Gwagwalada and the Immunization Unit of the Primary Health Care Centre, Gwagwalada, Abuja, Nigeria, over a period of 1 year (April 1, 2008-March 31, 2009). Appropriate ethical clearance was obtained from both institutions.
Subjects
Four categories of children of both sexes aged 0-2 years were recruited into the study after informed consent was obtained from their parents. There were 244 children with a complaint of fever only, 153 children with fever and diarrhea, 48 children with diarrhea only, and 285 apparently healthy children, who came to the health care facility for immunization, as controls. The axillary body temperatures of all the children were measured and temperatures above 37.2°C were taken as indicative of fever. Demographic characteristics of the children such as age, gender, and onset of the symptoms in the children were recorded. The presence of asexual forms of P. falciparum in a blood smear of a child with symptoms led to the diagnosis of uncomplicated clinical malaria. [7]
Collection of specimens and malaria parasite density determination
Blood specimens were obtained from deep finger pricks of all 730 children for the preparation of a thick blood film. The film slides were air-dried and stained with Field’s stains A and B and then examined under a light microscope using the oil immersions by an experienced microscopist. The number of parasites on each slide was calculated per 200 white blood cells (WBC) assuming 8000 WBC/μL of blood. [8] The level of parasitemia was designated as single (+) when 1-10 parasites were counted per 100 microscopic fields (mild/scanty parasitemia); or double (++) when 11-100 parasites were counted per 100 fields; or triple (+++) when 101-1000 parasites were counted per 100 fields. [8]
Statistical analysis
Data obtained were compared using the chi-square test with the SPSS statistical program. All reported P values were two-sided and P ≤ 0.05 was considered statistically significant.
| Results |
Of the 730 children admitted into the study, 337 (46.2%) were female and 393 (53.8%) male. Malaria parasites were detected in 75 (26.3%) of the apparently healthy children. Twelve afebrile children were found to have malaria parasites in their blood, while 161 (40.6%) of the children presenting with fever had malaria parasites in their blood [Table 1]. The prevalence of parasitemia among the febrile subjects was significantly higher than among the afebrile subjects, as indicated in [Table 2]. Two levels of parasitemia were observed among the study subjects. A total of 214 subjects had low level parasitemia (+) and 34 showed high level parasitemia (++) [Table 3]. The distribution of levels of parasitemia and symptomatic manifestation among the subjects in different age groups are shown in [Table 4].
| Table 1: Presence of malaria parasites among subjects
Click here to view |
| Table 2: Degree of parasitemia among subjects
Click here to view |
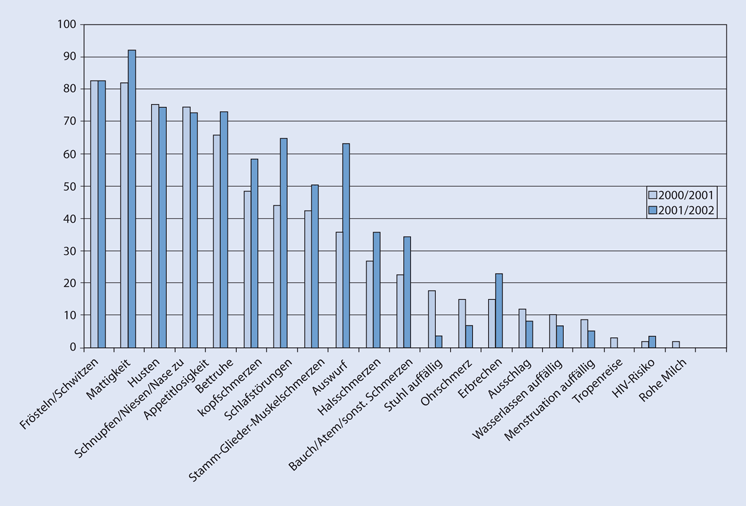 |
Table 3: Distribution of subjects after clinical diagnosis
Click here to view |
| Table 4: The distribution of levels of parasitemia and symptomatic manifestation among subjects in different age groups
Click here to view |
| Discussion |
The results of this study show that of the 397 children with a report of fever, only 161 (40.6%) had parasitemia, suggesting that in about 60% of cases of fever, malaria was not present. This revelation by microscopy that 60% of the febrile subjects had no parasitemia is an indication that a fever is not indicative of malaria parasitemia, suggesting that the treatment of all patients presenting with a fever with antimalarial drugs may be inappropriate. This observation is similar to other studies. [9],[10],[11] The WHO recommends that all patients, especially children, presenting at a health care facility with a history of fever in the past 24 h should be treated with antimalarial drugs. [12] The findings in this study suggest that the treatment of every febrile child with Coartem ® tablets [a fixed dose of the oral combination of artemether (20 mg) and lumefantrine (120 mg)], which has been shown to be effective in the treatment of chloroquine-resistant P. falciparum malaria, may be inappropriate. [13] As the use of antimalarial drugs is allowed by WHO for children aged under 5 years in malaria-endemic regions because of their vulnerability, the results of this study underscore the need to follow up the treatment with laboratory investigations and halting the treatment within 24 h if investigations cannot demonstrate the presence of malaria parasites. Apart from the problem of the development of antimalarial drug resistance, the wrong diagnosis in febrile aparasitemic patients may lead to an increase in the cost of hospital treatment and, more seriously, mortalities could occur, as the specific conditions responsible for their fever may go undetected and untreated.
The analysis of the density of parasitemia observed among the study subjects shows that most of the clinical malaria cases occurred in patients with low-level parasitemia. This suggests that most of the study subjects have a low immune status or have other underlying conditions that predispose them to clinical malaria even at a low parasite density.
Further analysis of the frequency of malaria among the study subjects showed that children aged 0-6 months had the lowest prevalence of malaria, followed by those aged 7-18 months. The children aged 19-24 months had a significantly higher prevalence of malaria than other age groups. The major difference between the children aged under 6 months and the others is that 67% of the youngest children were being breastfed, suggesting that the lower prevalence associated with these children could be the result of receiving protective antibodies from their mothers through breast milk. This observation is comparable to what has been observed in children with diarrhea who also derive a significant level of protection from diarrheal pathogens. [14]
Research carried out at the Department of Microbiology, La Trobe University has shown that various antibacterial, antiviral, and antiparasitic factors in human milk are active in vitro against a wide range of pathogens, which includes P. falciparum. In a study, breastfeeding was associated with a significantly lower risk of malaria in children 6-15 months old, while in children >15-24 months old, breastfeeding was not protective against malaria. [10] The finding in this study further underscores the need to continue counseling mothers to breastfeed their babies for as long as possible but not for less than 6 months.
The recorded prevalence of asymptomatic parasitemia among 26.1% of afebrile children is similar to the results from a previous study among Senegalese children aged less than 5 years, where a prevalence of 25.4% asymptomatic malaria parasitemia was observed. [15] This proportion of children, though small, is a significant potential source of malaria transmission. This parasitemia may, however, be due to a situation in which the children had not begun to exhibit malaria symptoms or might have been recovering from an attack. Furthermore, asymptomatic infections in areas of highly seasonal transmission may persist long enough through the dry season and reseed transmission when mosquito populations increase during the rainy season. [16] All these factors may be contributory to the difficulties in the correct diagnosis, control, and eradication of malaria in the malaria-endemic regions of the world.
| Conclusion |
The results of this study suggest that fever is not always indicative of malaria parasitemia and that subjects with asymptomatic infection must be regarded as a significant reservoir of transmissible malaria parasites within the study environment. It further suggests that breast milk appears to offer a significant level of protection against malaria parasites in young children.
| Acknowledgment |
We thank the management and staff of the Department of Medical Laboratory, University of Abuja Teaching Hospital, Gwagwalada, Federal Capital Territory, for their support and technical assistance in the collection and screening of the blood samples for malaria parasitemia.
| References |
| 1. |
Schaffner A. Fever-useful or noxious symptom that should be treated? Ther Umsch 2006;63:185-8.
|
| 2. |
Barone JE. Fever: Fact and fiction. J Trauma 2009;67:406-9.
|
| 3. |
Greenwood BM, Bojang K, Whitty CJ, Targett GA. Malaria. Lancet 2005;365:1487-98.
|
| 4. |
World Health Organization. Estimated Burden of Malaria in 2006. Geneva, World Malaria Report 2008; WHO/HTM/GMP/2008.1 ISBN 978 92 4 156369 7; p. 9 -12.
|
| 5. |
Lindblade KA, Steinhardt L, Samuels A, Kachur SP, Slutsker L. The silent threat: Asymptomatic parasitemia and malaria transmission. Expert Rev Anti Infect Ther 2013;11:623-39.
|
| 6. |
Breman JG. The ears of the hippopotamus: Manifestations, determinants, and estimates of the malaria burden. Am J Trop Med Hyg 2001;64(Suppl):1-11.
|
| 7. |
Smith TA. Measurement of clinical malaria in field trials of interventions against Plasmodium falciparum. Malar J 2007;6:53.
|
| 8. |
Cheesbrough M. District Laboratory Practice in Tropical countries Part 2. Cambridge CBZ ZRU, UK: Cambridge University Press; 2002. p. 136-142, 320-9.
|
| 9. |
Mazigo HD, Meza W, Ambrose EE, Kidenya BR, Kweka EJ. Confirmed malaria cases among children under five with fever and history of fever in rural western Tanzania. BMC Res Notes 2011;4:359.
|
| 10. |
Vora N, Homsy J, Kakuru A, Arinaitwe E, Wanzira H, Sandison TG, et al. Breastfeeding and the risk of malaria in children born to HIV-infected and uninfected mothers in rural Uganda. J Acquir Immune Defic Syndr 2010;55:253-61.
|
| 11. |
Olaleye BO, Williams LA, D’Alessandro U, Weber MM, Mulholland K, Okorie C, et al. Clinical predictors of malaria in Gambian children with fever or a history of fever. Trans R Soc Trop Med Hyg 1998;92:300-4.
|
| 12. |
World Health Organization. Policies, strategies and targets for malaria control. Geneva, World Malaria Report 2008; WHO/HTM/GMP/2008.1 ISBN 978 92 4 156369 7; pp. 25-9.
|
| 13. |
Falade CO, Ogunkunle OO, Dada-Adegbola HO, Falade AG, de Palacios PI, Hunt P, et al. Evaluation of the efficacy and safety of artemether-lumefantrine in the treatment of acute uncomplicated Plasmodium falciparum malaria in Nigerian infants and children. Malar J 2008;7:246.
|
| 14. |
Onanuga A, Igbeneghu O, Lamikanra A. A study of the prevalence of diarrhoeagenic Escherichia coli in children from Gwagwalada, Federal Capital Territory, Nigeria. Pan Afr Med J 2014;17:146.
|
| 15. |
Le Port A, Cot M, Etard JF, Gaye O, Migot-Nabias F, Garcia A. Relation between Plasmodium falciparum asymptomatic infection and malaria attacks in a cohort of Senegalese children. Malar J 2008;7:193.
|
| 16. |
Babiker HA, Abdel-Muhsin AM, Ranford-Cartwright LC, Satti G, Walliker D. Characteristics of Plasmodium falciparum parasites that survive the lengthy dry season in eastern Sudan where malaria transmission is markedly seasonal. Am J Trop Med Hyg 1998;59:582-90.
|
Source of Support: This work was not supported by any agencies or institutions,, Conflict of Interest: None
| Check |
DOI: 10.4103/1755-6783.156668
| Tables |
[Table 1], [Table 2], [Table 3], [Table 4]



